Epidemiology of Non-Hodgkin's Lymphoma.
Study Design
- Çalışma Türü
- Review
- Popülasyon
- None
- Müdahale
- Epidemiology of Non-Hodgkin's Lymphoma. None
- Karşılaştırıcı
- None
- Birincil Sonuç
- None
- Etki Yönü
- Mixed
- Yanlılık Riski
- Unclear
Abstract
Non-Hodgins's lymphoma (NHL) is the most common hematological malignancy worldwide, accounting for nearly 3% of cancer diagnoses and deaths. NHL is the seventh most prevalent cancer and has the sixth highest mortality among cancers in the US. NHL accounts for 4% of US cancer diagnoses, and incidence has increased 168% since 1975 (while survival has improved 158%). NHL is more common among men, those >65 years old, and those with autoimmune disease or a family history of hematological malignancies. NHL is a heterogenous disease, with each subtype associated with different risk factors. Marginal zone lymphoma (MZL) is strongly associated with Sjogren's syndrome (SS) and Hashimoto's thyroiditis, while peripheral T-cell lymphoma (PTCL) is most associated with celiac disease. Occupational exposures among farm workers or painters increases the risk of most of the common subtypes. Prior radiation treatment, obesity, and smoking are most highly associated with diffuse large B-cell lymphoma (DLBCL), while breast implants have been rarely associated with anaplastic large cell lymphoma (ALCL). Infection with Epstein-Barr Virus (EBV) is strongly associated with endemic Burkitts lymphoma. HIV and human herpes virus 8 (HHV-8), is predisposed to several subtypes of DLBCL, and human T-cell lymphoma virus (HTLV-1) is a causative agent of T-cell lymphomas. Obesity and vitamin D deficiency worsen NHL survival. Atopic diseases and alcohol consumption seem to be protective against NHL.
Kısaca
Non-Hodgins’s lymphoma (NHL) is the most common hematological malignancy worldwide, accounting for nearly 3% of cancer diagnoses and deaths and incidence has increased 168% since 1975 (while survival has improved 158%).
Full Text
medical sciences
Review
Epidemiology of Non-Hodgkin’s Lymphoma
Krishna C. Thandra 1,*, Adam Barsouk 2, Kalyan Saginala 3, Sandeep Anand Padala 4 , Alexander Barsouk 5 and Prashanth Rawla 6
- 1 Department of Pulmonary and Critical Care Medicine, Sentara Virginia Beach General Hospital, Virginia Beach, VA 23455, USA
- 2 Sidney Kimmel Cancer Center, Jefferson University, Philadelphia, PA 19107, USA; [email protected]
- 3 Plains Regional Medical Group Internal Medicine, Clovis, NM 88101, USA; [email protected]
- 4 Department of Medicine, Nephrology, Medical College of Georgia, Augusta University, Augusta, GA 30912, USA; [email protected]
- 5 Hematologist-Oncologist, Allegheny Health Network, Pittsburgh, PA 15212, USA; [email protected]
- 6 Department of Medicine, Sovah Health, Martinsville, VA 24112, USA; [email protected]
* Correspondence: [email protected]; Tel.: +1-757-481-2515
Citation: Thandra, K.C.; Barsouk, A.; Saginala, K.; Padala, S.A.; Barsouk, A.; Rawla, P. Epidemiology of Non-Hodgkin’s Lymphoma. Med. Sci. 2021, 9, 5. https://doi.org/ 10.3390/medsci9010005
Received: 28 December 2020 Accepted: 27 January 2021 Published: 30 January 2021
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Copyright: © 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https:// creativecommons.org/licenses/by/ 4.0/).
Abstract: Non-Hodgins’s lymphoma (NHL) is the most common hematological malignancy worldwide, accounting for nearly 3% of cancer diagnoses and deaths. NHL is the seventh most prevalent cancer and has the sixth highest mortality among cancers in the US. NHL accounts for 4% of US cancer diagnoses, and incidence has increased 168% since 1975 (while survival has improved 158%). NHL is more common among men, those >65 years old, and those with autoimmune disease or a family history of hematological malignancies. NHL is a heterogenous disease, with each subtype associated with different risk factors. Marginal zone lymphoma (MZL) is strongly associated with Sjogren’s syndrome (SS) and Hashimoto’s thyroiditis, while peripheral T-cell lymphoma (PTCL) is most associated with celiac disease. Occupational exposures among farm workers or painters increases the risk of most of the common subtypes. Prior radiation treatment, obesity, and smoking are most highly associated with diffuse large B-cell lymphoma (DLBCL), while breast implants have been rarely associated with anaplastic large cell lymphoma (ALCL). Infection with Epstein–Barr Virus (EBV) is strongly associated with endemic Burkitts lymphoma. HIV and human herpes virus 8 (HHV-8), is predisposed to several subtypes of DLBCL, and human T-cell lymphoma virus (HTLV-1) is a causative agent of T-cell lymphomas. Obesity and vitamin D deficiency worsen NHL survival. Atopic diseases and alcohol consumption seem to be protective against NHL.
Keywords: NHL; non-Hodgkin’s lymphoma; epidemiology; incidence; prevalence; mortality; prevention; risk factors
1. Introduction
Non-Hodgins’s lymphoma (NHL), the most common hematological malignancy worldwide, refers to a diverse class of B-cell and T-cell proliferations. NHL is differentiated from Hodgkin’s lymphoma by different clinical characteristics and the absence of Reed–Sternberg cells and Cd15 and Cd30 staining on histology. While there are over 40 major subtypes, the most common types include indolent follicular lymphoma (FL) and aggressive diffuse large B-cell lymphoma (DLBCL). Each type is associated with unique driver genetic mutations (e.g., 14:18 translocation in FL, 11:14 translocation in Mantle Cell, 8:14 in Burkitts lymphoma ) and unique risk factors (Epstein–Barr Virus (EBV) for Burkitt’s lymphoma, human T-cell lymphoma virus (HTLV-1) for T-cell lymphoma) [1]. Population-based cancer registries, such as those compiled in the 2018 GLOBOCAN, do not distinguish NHL subtypes based on the extensive WHO classifications, making global epidemiological data on NHL subtypes limited [2]. Due to the heterogeneity of NHL, the International Lymphoma Epidemiology Consortium (InterLymph) was established in 2001 to elucidate subtype-specific risk factors and disease mechanisms [3]. Global epidemiology
Med. Sci. 2021, 9, 5. https://doi.org/10.3390/medsci9010005 https://www.mdpi.com/journal/medsci
statistics as well as common risk factors identified by InterLymph, based on meta-analysis data, are summarized below.
2. Epidemiology 2.1. Incidence
According to the latest GLOBOCAN data, an estimated 509,600 new cases of NHL were diagnosed globally in 2018, comprising 2.8% of worldwide cancer diagnoses. The global age standardized risk of NHL was 6.7 among men and 4.7 among women, translating to a 0.72% and 0.35% cumulative lifetime risk for men and women, respectively. The incidence in high and low/medium human development index nations, respectively, was 7.8/100,000 and 4.3/100,000 among men and 5.6/100,000 and 2.9/100,000 among women (Figure 1) [4].
- Figure 1. Bar chart showing estimated age-standardized incidence and mortality rates (World) in 2018, non-Hodgkin’s lymphoma, all sexes, all ages. Data obtained from Globocan 2018.
According to the latest World Health Organization (WHO) classification, the most common NHL in Western countries is DLBCL, accounting for around 31% of adult cases. Other common aggressive B-cell subtypes include Mantle Cell Lymphoma (MCL) (6% of cases) and BL (2% of cases). Among indolent B-cell NHL, FL accounts for 22% of cases in the Western world, followed by marginal zone lymphoma (MZL) (8% of cases), chronic lymphocytic leukemia/small-cell lymphocytic lymphoma (CLL/SLL) (6% of cases) and lymphoplasmacytic lymphoma (LPL) (1% of cases). Common T-cell lymphomas make up only 10–15% of NHL diagnoses and include peripheral T-cell lymphoma (PTCL) (6% of cases) and cutaneous T-cell lymphoma (CTCL) (4% of cases) [1].
An estimated 77,200 new cases of NHL were diagnosed in 2020 in the US, accounting for 4.3% of cancer diagnoses (the seventh most common cancer diagnosis). The most recent reported incidence was 18.6/100,000 in 2017, a 168% increase from the earliest reported incidence of 11.1/100,000 in 1975 [5]. Figure 2 shows age-standardized incidence rates for NHL worldwide in 2018.
2.2. Mortality
An estimated 248,700 global deaths were attributable to NHL in 2018 (See Figure 3), accounting for 2.6% of all oncological mortality. Men had a 0.33% cumulative lifetime risk of NHL mortality, while the risk for women was estimated at 0.21%. The mortality in both
high and low/medium HDI nations was 3.2/100,000 among men, and 2.0/100,000 and
- 1.9/100,000 among women, respectively [4].
- Figure 2. Map showing estimated age-standardized incidence rates (ASR) for non-Hodgkin’s lymphoma worldwide in 2018, all sexes, including all ages. Created with mapchart.net. Data obtained from Globocan 2018.
- Figure 3. Map showing estimated age-standardized mortality rates (ASR) for non-Hodgkin’s lymphoma worldwide in 2018, all sexes, including all ages. Created with mapchart.net. Data obtained from Globocan 2018.
The mortality in the US was an estimated 19,900 in 2020, accounting for 3.3% of all cancer deaths (making NHL the sixth leading cause of oncological mortality). The most
recent reported mortality was 5.1/100,000 in 2018, down from a peak of 8.9/100,000 in 1997. The death rate was for men was 7.0/100,000, significantly greater than the 4.1 reported in women [5].
- 2.3. Survival
- 3. Non-Modifiable Risk Factors Table 1 indicates modifiable and non-modifiable risk factors.
- Table 1. Modifiable and non-modifiable risk factors.
Non-Modifiable Risk Factors Modifiable Risk Factors
Age Radiation
Gender Chemical Exposure Race/Ethnicity Obesity Family History Tobacco smoking and alcohol
Autoimmune Diseases Breast Implants Immunosuppression Vitamin Deficiency
- 3.1. Age
- 3.2. Gender
- 3.3. Race/Ethnicity
In the US, white and non-Hispanic people are at highest risk of NHL, while Asian/Pacific Islander, American Indian and black populations are at the lowest risk. The incidence out of 100,000 was 25.0 and 17.0 in white men and women, respectively, compared to 10.8 and 10.9 among American Indians, 16.5 and 11.1 in Asian/Pacific Islanders, 17.7 and 12.5 in African Americans, and 20.9 and 15.9 in Hispanics [5]. However, the T-cell lymphoma mycosis fungoides shows higher incidence among African Americans [3]. East Asian nations, in particular Japan, as well as nations in West Africa and the Caribbean, have higher rates of human T-cell lymphoma virus (HTLV-1), and subsequently higher incidence of T cell lymphoma. Similarly, children in subequatorial Africa are at higher risk of endemic Burkitt Lymphoma from Epstein–Barr Virus (EBV), with an interplay with malaria infection suspected. The discrepancies in viral NHL risk across ethnicities and geography remains unelucidated [6].
- 3.4. Family History
- 3.5. Autoimmune Diseases
- 3.6. Immunosuppression
Certain subtypes of NHL have been associated with immunosuppressive conditions. The immunodeficiency associated subtype of BL has been highly associated with human immunodeficiency virus (HIV) and solid organ transplant [14]. Among those with organ transplants in the US, the risk of BL is 23× higher, in part due to increased risk of infection with EBV. The risk is likewise heightened for those undergoing immunosuppressive therapies for autoimmune diseases [16].
4. Modifiable Risk Factors
- 4.1. Radiation
- 4.2. Chemical Exposure
Exposure to various occupational chemicals and tobacco has been linked with several subtypes of NHL. Working on a farm or as a painter is associated with an increased risk of NHL (OR = 1.28, 1.22, respectively) [15]. For DLBCL in particular, working on a farm (OR = 1.78), as a seamstress and embroider (OR = 1.49), hairdresser (OR = 1.65), or equipment operator/driver (OR = 1.58), in particular mediastinal DLBCL [7]. Working as a spray painter was associated with FL with an OR of 2.66 [9]. Certain subtypes of PTCL are associated with a >40-year history of smoking (OR = 1.76), working with electrical fitters (OR = 4.08 for anaplastic large cell lymphoma (ALCL) and OR = 5.45 for angioimmunoblastic T-cell lymphoma (AITL)), or working with textiles (OR = 2.60 for ALCL) [13]. Mycosis fungoides, the most common type of cutaneous T-cell lymphoma, was associated with working in farming (OR = 2.37), painting (OR = 3.71), woodworking (OR = 2.20), or carpentering (OR = 4.07) [19,20].
- 4.3. Obesity
- 4.4. Tobacco Smoking and Alcohol
- 4.5. Breast Implants
- 4.6. Vitamin D Deficiency
Increased sun exposure was shown to decrease the risk of DLBCL, FL, CLL/SLL and ALCL, likely by stimulating production of vitamin D3, a potent immune modulator [24]. However, vitamin D supplementation did not significantly affect NHL risk in a metaanalysis [25]. Higher vitamin D levels were associated with improved lymphoma survival among Norwegian patients [26], and higher vitamin D levels at diagnosis decreased cancer fatality rates (HR = 0.59) after a mean 14.4 year follow-up time [27]. Studies from other nations also found that vitamin D deficiency was associated with inferior survival in CLL/SLL [28], DLBCL, and T-cell lymphoma [29]. A randomized control study at the Mayo clinic investigating vitamin D as a chemotherapy adjunct for NHL is currently recruiting.
- 5. Infections Table 2 below indicates subtypes of NHL associated with various infections.
- Table 2. Subtypes of non-Hodgkin’s lymphoma (NHL) associated with infections.
Infection Sub Types of NHL
EBV Burkitt’s lymphoma HIV DLBCL, Primary brain lymphoma
HTLV-1 DLBCL HHV-8 Primary effusion lymphoma
Hepatitis C DLBCL Helicobacter Pylori MALT
- 5.1. Epstein–Barr Virus (EBV)
EBV, also known as HHV-4, is strongly associated with endemic BL, which most often presents as a jaw-lesion (or kidney) on children in developing nations. In studies in Egypt and Brazil, 87% of BL patients were found to be EBV positive. EBV was also found to account for 74% of all childhood malignancies in subequatorial Africa. EBV increases the risk of MYC translocation from chromosome 8 to an immunoglobulin locus on chromosome 14, rendering the oncogene constitutively active [30].
- 5.2. Human Immunodeficiency Virus (HIV)
- 5.3. Human T-Cell Lymphotropic Virus (HTLV-1)
- 5.4. Human Herpes Virus 8 (HHV-8)
- 5.5. Hepatitis C
- 5.6. Helicobacter Pylori
Gastric (MALT-gastric mucosa-associated lymphoid tissue) lymphoma is a form of non-Hodgkin’s lymphoma affecting the stomach. There is limited evidence available, but available case-control studies showed association of H. pylori infection and gastric non-Hodgkin’s lymphoma with odds ratio of 6.3%. Eradication of H. pylori with therapy was associated with high rates of remission of the MALT lymphoma [36].
6. Conclusions
NHL is a heterogenous group of diseases which constitute the most commonly diagnosed hematological malignancy worldwide, comprising nearly 3% of all cancer diagnoses. In the US, NHL is the seventh most common and sixth most deadly malignancy. NHL is more common among men >65 years old of European and Hispanic descent. While survival has improved in the Western world with new therapeutics, prevention measures aimed at the diverse array of NHL risk factors could significantly reduce the global cancer burden. In particular, reducing chemical exposure in the workplace, tobacco smoking, obesity, and transmission of viruses such as HIV, EBV, HTLV-1 and HCV, and increasing sun exposure and vitamin D supplementation, are strong targets for public health initiatives aimed at NHL prevention.
Author Contributions: Conception and design, K.C.T., A.B. (Adam Barsouk) and K.S.; analysis and interpretation, drafting and critical revision of the article, A.B. (Adam Barsouk), K.S., K.C.T., S.A.P., A.B. (Alexander Barsouk) and P.R; final approval of the article, K.C.T., A.B. (Adam Barsouk), K.S., S.A.P., A.B. (Alexander Barsouk) and P.R. All authors have read and agreed to the published version of the manuscript.
Funding: This research received no external funding. Conflicts of Interest: The authors declare no conflict of interest.
Figures
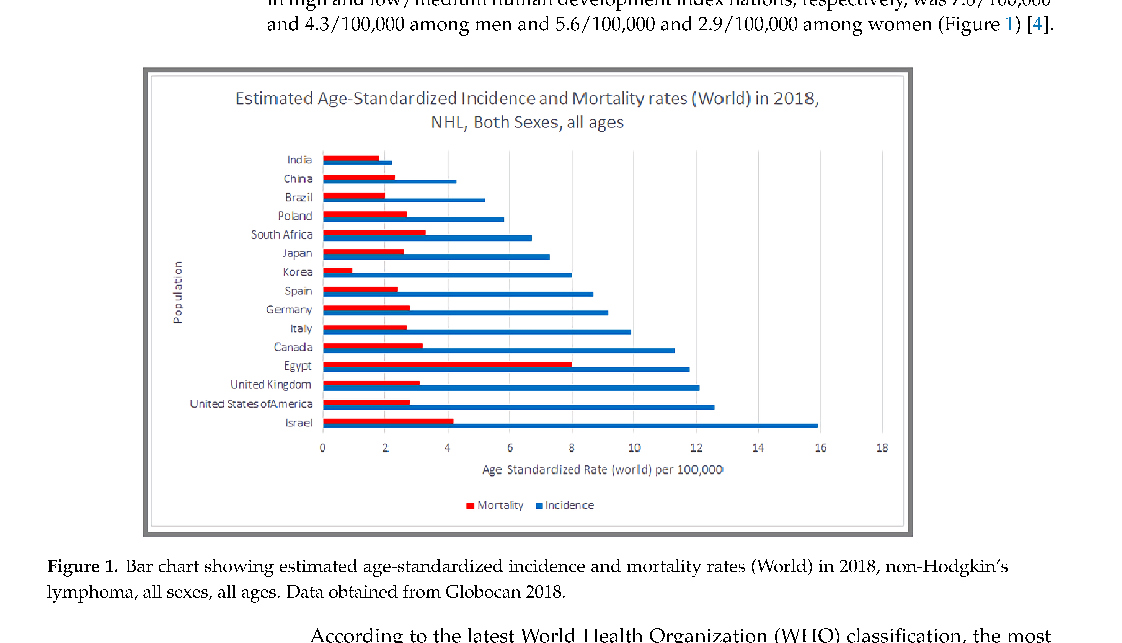
Figure 6
NHL mortality patterns reflect disparities in treatment access and disease subtype distribution. This figure presents survival and mortality data across different NHL classifications.
chart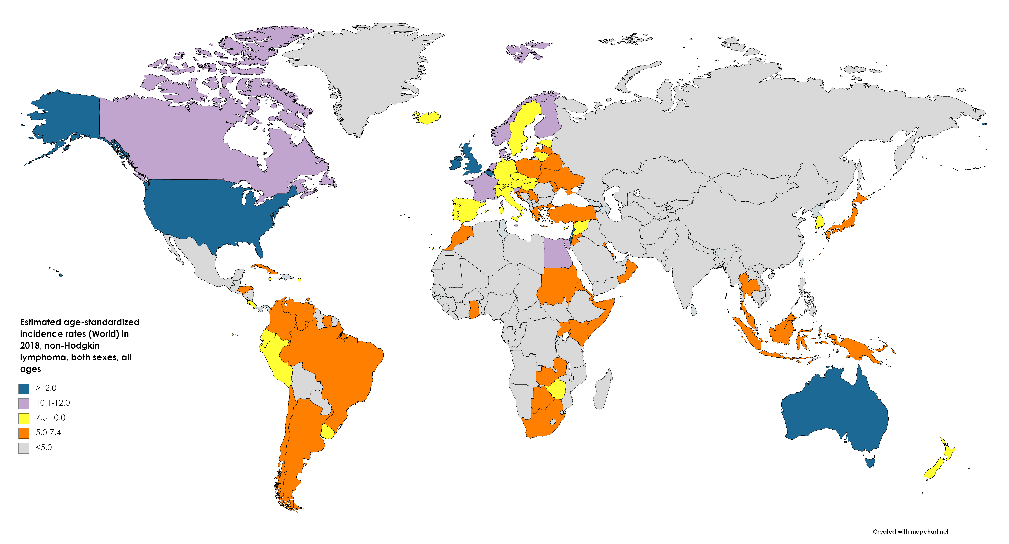
Figure 7
The epidemiological profile of Non-Hodgkin's lymphoma continues to evolve with improved molecular classification. This figure provides additional epidemiological data on NHL subtypes and their relative frequencies.
chartUsed In Evidence Reviews
Similar Papers
Archives of internal medicine · 2009
Association between serum 25-hydroxyvitamin D level and upper respiratory tract infection in the Third National Health and Nutrition Examination Survey.
Journal of autoimmunity · 2019
Systemic lupus erythematosus: Diagnosis and clinical management.
Journal of investigative medicine : the official publication of the American Federation for Clinical Research · 2011
Vitamin D and the immune system.
Archives of disease in childhood · 2021
Why is COVID-19 less severe in children? A review of the proposed mechanisms underlying the age-related difference in severity of SARS-CoV-2 infections.
Gastroenterology · 2010
Primary prevention of colorectal cancer.
Journal of cachexia, sarcopenia and muscle · 2020